A new article published in Clinical Lactation addresses potential negative outcomes of epidurals and other birth interventions. Birth Interventions Related to Lower Rates of Exclusive Breastfeeding and Increased Risk of Postpartum Depression in a Large Sample, was written by Kathleen Kendall-Tackett, PhD, IBCLC, FAPA, Zhen Cong, PhD, and Thomas W. Hale, PhD.
 Kendall-Tackett, Cong, and Hale specifically examined the effects of birth interventions on exclusive breastfeeding and postpartum depression using data from the Survey of Mothers’ Sleep and Fatigue, a study of 6,410 new mothers from 59 countries. They found that epidurals were associated with lower exclusive breastfeeding rates and higher rates of postpartum depression even after controlling for other factors that increase mothers’ risk of depression, such as history of depression and sexual assault; income and education level; and the other birth interventions. In addition, mothers were more likely to be depressed if they perceived their labors as very painful and difficult, and if they had postpartum complications, such as hemorrhage or surgery. These findings contradict previous studies that found that birth interventions, particularly epidurals, had no negative effect on maternal mental health or breastfeeding. According to Dr. Kendall-Tackett, this current study is important because the sample size is large enough to allow the researchers to control for many of the factors that could account for mothers’ depression.
Kendall-Tackett, Cong, and Hale specifically examined the effects of birth interventions on exclusive breastfeeding and postpartum depression using data from the Survey of Mothers’ Sleep and Fatigue, a study of 6,410 new mothers from 59 countries. They found that epidurals were associated with lower exclusive breastfeeding rates and higher rates of postpartum depression even after controlling for other factors that increase mothers’ risk of depression, such as history of depression and sexual assault; income and education level; and the other birth interventions. In addition, mothers were more likely to be depressed if they perceived their labors as very painful and difficult, and if they had postpartum complications, such as hemorrhage or surgery. These findings contradict previous studies that found that birth interventions, particularly epidurals, had no negative effect on maternal mental health or breastfeeding. According to Dr. Kendall-Tackett, this current study is important because the sample size is large enough to allow the researchers to control for many of the factors that could account for mothers’ depression.
“The majority of previous studies found that epidurals did not negatively affect either breastfeeding or maternal mental health. However, most of those studies were severely limited by small sample sizes. Our study has one of the largest samples to date and accounts for many of the other factors that put women at risk for depression. The significance of our study is that even after we controlled for all these other factors, epidurals still increased risk for depression. For an individual mother, having an epidural can be the right choice. But we should not assume that that choice has no consequence. It does. We should be sure to monitor mothers who have epidurals for signs of either breastfeeding difficulties or depressive symptoms.”
Dr. Kendall-Tackett, author of Depression in New Mothers, 2nd Edition (Routledge), is a health psychologist and International Board Certified Lactation Consultant. She is a Fellow of the American Psychological Association in Health and Trauma Psychology, a Clinical Professor of Nursing at the University of Hawaii at Manoa, and Clinical Associate Professor of Pediatrics at the Texas Tech University School of Medicine in Amarillo, Texas. Dr. Kendall-Tackett is Editor-in-Chief at Praeclarus Press is a small press that specializes in women’s health based in Amarillo, Texas. Dr. Cong is Associate Professor of Human Development and Family Studies at Texas Tech University in Lubbock, Texas. Dr. Hale is Professor of Pediatrics at Texas Tech University School of Medicine in Amarillo, Texas and Director of the InfantRisk Center at Texas Tech.
How Birth Trauma Impacts Breastfeeding – With Kathleen Kendall-Tackett
Breastfeeding expert, Kathleen Kendall-Tackett, PhD, shares the latest research that shows a greater number of women suffer from post traumatic stress disorder, PTSD, after giving birth than downtown Manhattan survivors suffered PTSD after the terrorist attack on the World Trade Centers on 9-11. Women suffer from birth trauma that rises to the level of diagnosable PTSD at a rate of 9%, while 9-11 survivors using the same criteria were 7.5%, states Kendall-Tackett in the video.
In this interview with Lisa Reagan, Kindred’s editor, Kendall-Tackett spells out the reasons for PTSD not being recognized in birth until recent years, and the even more recent revelations of the impact of birth trauma on breastfeeding. See the entire playlist of Kendall-Tackett videos on Kindred’s New Story YouTube Channel here.
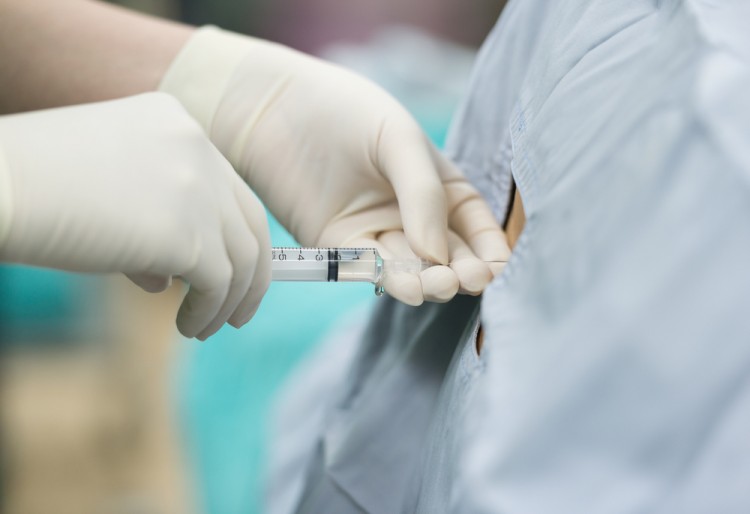
Featured photo Shutterstock/ChaNaWiT



Thank you for this important report. I work as a psychologist with perinatal mood disorders. Is it possible to receive a copy of the original research study publication so I can share with my colleagues? Thank you in advance.
Please, let us not forget that the natural birth movement was about women having a voice in their health care. I fear we have lost sight of that and are trending toward a culture of guilt and shame when women choose or need birth interventions. Ultimately the greatest predictor of birth trauma and resulting PPD is the woman’s sense of being informed and supported and in control through it all.
I agree with your comment in the sense that no woman should be shamed or looked down because she needed or wanted intervention.
But what this study shows is that the use of epidurals and other interventions is directly linked with PTSD and PPD after their use.
It is a simple fact, in the same way that feeling tired and overwhelmed may cause someone to drink 2 bottles of wine, sleep heavily and wake up hung over and depressed. It’s just something that happens. If you had dear friends or family drinking wine with you, and you woke up the next morning feeling hung over and awful, but someone sweet and supportive woke up next to you, and laughed with you about what a bad idea it was, and brought you water and coffee and juice and eggs and toast, and then let you sleep and recover a bit, your feeling of depression and regret wouldn’t be nearly as bad.
Or better still, if you skipped the wine completely, cried with your friends and family, had them there to support and hold you through your difficult night, you would quite possibly wake up feeling better, with strength, energy and positivity for the new day. This is not a very good analogy for birth, I know, but bear with me.
Women who are scared, unsupported, not given enough info by their care providers, forced to labour in uncomfortable positions, and who are made to feel weak and out of control about their own birth, experience way more pain and stress, and often the only coping strategy they have is an epidural, or cocaine/opiate based drugs.
Women who go into birth with good education, a good understanding of what is available to them, and a supportive team of doctor/midwife, doula, well prepared partner, caring family, etc , may still have an epidural or other intervention, but when you have been respected and informed and given time and options, the negative effects can be much less.
Those who appear to be trying to shame women into not having epidurals or interventions are often simply suggesting the third option: let’s scrap the 2 bottles of wine completely and rather give you a humane and gentle care provider, an experienced doula, a well prepared and empowered partner, the option of family or friends to support you as well, an optimal environment for birth: privacy, darkness, warmth, safety, no ticking clocks, a deep pool of hot water, soft hands and kind words…will you still need an epidural then? When your mind is calm and your body is comfortable? When your heart is ready, when your adrenaline is low and your oxytocin is high? When YOU are the one deciding how and when to bring your child into the world?
When we make the conditions under which women give birth more mammalian, more human, more autonomous, the need for interventions will be extremely low, as it should be. And those who do have interventions will know that they really, really needed them, and hopefully they will be watched closely and given strong support and help through the “hangover” which comes after. Not shamed or left alone or ignored.
‘Sudden, injurous and overwhelming’. This is very helpful in watching out for PTSS in new mothers. Thank you for your work in pointing out this commonality. And for the link between traumatic birth and sub-optimal lactation. Women do experience these things and now, having the evidence will be helpful in explaining to women why they feel as they do. Hopefully it’ll help allay their guilt which tends to accompany PTSS.